Calcific Tendonitis
The rotator cuff is a group of four muscles and their tendons that attach around the top of the arm bone (humerus) forming a ‘hood’. The rotator cuff holds the ball in the socket providing stability and mobility. By keeping the ball in the socket, it allows the outer muscle (deltoid) to move the shoulder joint in a co-ordinated way.
 Above the rotator cuff is a shelf of bone (acromion) which is an extension of the shoulder blade (scapula). This acromion forms a joint (acromioclavicular joint; ac joint) with the end of the collarbone (clavicle). Between the rotator cuff and the acromion there is a bursa or cushion of fluid, which allows for smooth movement when the rotator cuff moves against the acromion as the arm is lifted up. Soft tissue thickening or bony prominences (spurs) under the acromion and acromioclavicular joint can result in irritation of the rotator cuff as it moves under and against the acromion.
Above the rotator cuff is a shelf of bone (acromion) which is an extension of the shoulder blade (scapula). This acromion forms a joint (acromioclavicular joint; ac joint) with the end of the collarbone (clavicle). Between the rotator cuff and the acromion there is a bursa or cushion of fluid, which allows for smooth movement when the rotator cuff moves against the acromion as the arm is lifted up. Soft tissue thickening or bony prominences (spurs) under the acromion and acromioclavicular joint can result in irritation of the rotator cuff as it moves under and against the acromion.
Would you like to see a doctor?
Learn more
Rotator Cuff Calcification
Calcium can occur in the rotator cuff tendons. The reason why calcium is deposited there is uncertain but it is most likely due to degeneration or wear and tear in the tendons – the body then deposits calcium there as a reparative process.
Calcium can cause pain from inflammation within the calcium or inflammation in the tendon around the calcium.
The presence of the calcium makes the tendon a little thicker and this in turn may lead to inflammation of the rotator cuff as it moves against the shelf of bone (acromion) when the arm is lifted up. This process is called ROTATOR CUFF IMPINGEMENT.
Acute Calcific Tendonitis
Calcium can be present in 2 forms either as a chalk-like solid or like toothpaste. In some instances the calcium can become acutely swollen and behave like an abscess causing severe acute pain in the shoulder. This pain may limit the patient from sleeping and lifting the arm from the side. This can be the most severe pain felt in the shoulder. At times the calcium may burst into the space above the rotator cuff tendons resulting in spontaneous resolution. This almost invariably responds to injection.
Diagnosis
How is the diagnosis made?
This is made from the history and examination. Pain is the most common presenting complaint and is usually sited over the shoulder joint itself and can radiate down the arm, into the neck or into the shoulder blade. Some patients only feel the pain over the midpart of the arm with no pain felt in the shoulder itself. Pain is related to movements of the shoulder and in particular movements with the arm overhead, behind the back, when stretching out or when lifting anything heavy. Most patients feel the pain at night, which disturbs their sleep and can be very distressing. Patients may feel that the arm is weak. The examination is aimed at reproducing the pain and testing the strength of the rotator cuff muscles. X-rays are taken which will usually show the presence of calcium but this may also be seen with the use of ultrasound. What is the treatment?
Treatment
Non Operative Treatment
Subacromial injection of local anaethetic and cortisone or actual needling/aspiration of the calcium under ultrasound guidance. Needling is done in the rooms under local anaesthetic; this is successful in about 2/3rds of patients but the paradox is that even when no calcium is sucked out, there can be complete resolution and vice versa. i.e. when a large amount of calcium comes out there may not be complete resolution.
PHYSIOTHERAPY
Physio is aimed at stretching exercises to loosen up the capsule or lining of the joint. Strengthening of the rotator cuff muscles and the muscles that stabilse and move the scapula ( shoulder blade).
Tightness of the back of this capsule is implicated in the causation of impingement. Tightness of the posterior capsule leads to the ball or humeral head being pushed forward which results in impingement when the arm is elevated. Stretching of the back of the capsule is important in helping resolve it.
This is done in the following ways:
 Standing or sitting.
Standing or sitting.
Take the hand of you affected arm across your body towards the opposite shoulder.
Give gentle assistance with your other arm.
Repeat 10 to 30 times and do 2 to 3 times a day.
Strengthening of the Rotator Cuff Muscles
The function of the rotator cuff muscles is to stabilise and mobilise the shoulder. They keep the ball (humeral head) in the socket. If there is any weakness of the rotator cuff muscles then the humeral head may move slightly abnormally resulting in rotator cuff impingement. Strengthening of the rotator cuff muscles will help prevent or resolve impingement.
This is done by strengthening the muscles that turn the arm outwards (external rotation) and the muscles that turn the arm inwards (internal rotation)
STRENGTHENING OF EXTERNAL ROTATION
Sitting or standing with your elbow bent.
Keep your elbow INTO your side.
Hold one end of elastic band – other end fixed.
Start with your hand in front of your stomach and pull hand outwards until it is in front of you.
CONTROL the movement on return and do NOT try and pull out too far.
Repeat 30 times
 STRENGTHENING OF INTERNAL ROTATION
STRENGTHENING OF INTERNAL ROTATION
Shown for the right arm
Stand with arm close to your body and elbow bent.
Hold rubber elastic band – other end of band fixed.
Pull your hand towards your stomach.
Keep the elbow in.
Control the movement on return.
Repeat 30 times.
Strengthening of internal and external rotation can be done with dumbbells in the following way:
 STRENGTHENING WITH DUMBBELL – External Rotation
STRENGTHENING WITH DUMBBELL – External Rotation
 STRENGTHENING WITH DUMBBELL – Internal Rotation
STRENGTHENING WITH DUMBBELL – Internal Rotation
Repeat 30 times
Strengthening of the Scapular muscles
Stengthening of the scapular muscles which control the position and movement of the shoulder blade is important.
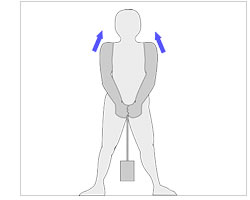
With your feet 3 feet apart and keeping the elbows straight, adjust the rope so the weight is just resting on the ground.
Now shrug your shoulders so the weight is lifted off the ground.
With your feet 2 feet apart and hands on the wall in front, bend your elbows till your face almost touches the wall.
Start with doing 10 repetitions and then moving to do 30 repetitions.
You should do all these exercises 2 to 3 times per day.
Surgery & Post-Surgery Exercises
SURGERY
This is indicated when the condition has been present for over +/- 6 months and has not responded to up to 3 injections or needlings. In acute calcific tendinitis, surgery may be indicated early if the severe pain does not settle after injection.
Surgery involves needling of the calcium under direct vision. Additionally some bone is shaved from the undersurface of the acromion to increase the ‘space’ between the tendons and acromion. The end of the collarbone (clavicle) may need to be removed if it has been identified as a source of pain.
This is done with ARTHROSCOPY or ‘key hole surgery’
See video clips below:
A NEEDLE IS USED TO MAKE A SMALL INCISION (5mm) IN THE ROTATOR CUFF TENDON AND A PROBE IS USED TO HELP EXTRACT THE CALCIUM.
VIDEOS
EXERCISES AFTER THE OPERATION
Use pain-killers and/or ice packs to reduce the pain before you exercise.
Do short frequent sessions (eg: 5-10 minutes, 4 times a day) rather than one long session.
It is normal to feel aching, discomfort or stretching sensations when doing these exercises.
However, intense and lasting the pain (ie: > 30 minutes) is an indication to change the exercise by doing it less forcefully or less often. Continue to do these exercises until you get the movement back, or you see the physiotherapist.
Lean forwards, let your arm hang freely.
Start with small movements.
Swing your arm: forwards & backwards side to side in circles
Repeat each movement 5 times
Sitting or standing, elbow to your side.
Hand near stomach.
Take hand away from stomach. (This twists the shoulder joint.)
Can support/add pressure with a stick held between your hands.
Repeat 10 times.
 FLEXION IN LYING
FLEXION IN LYING
Lying on your back on bed/ floor.
Support your operated arm and lift up overhead.
Gradually remove the support.
Then progress to trying the movement sitting or standing.
Repeat 10 times.
Frequently Asked Questions
Do I need to do exercises?
Yes! You will be shown exercises by the physiotherapist in the hospital the day after the operation and you will need to continue with the exercises once you go home. They aim to stop your shoulder getting stiff and to strengthen the muscles around your shoulder. The early exercises are shown at the back of this booklet. The physiotherapist will arrange an appointment to see you as an outpatient or will refer you back to your own physio. However you may start using the arm as pain permits.
What do I do about the wound?
Waterproof dressing will be applied to the small wounds on the day after the operation and you will be able to wash and shower with these on. Avoid using spray deodorant, talcum powder or perfumes near or on the wounds until they are well healed.
When will I be reviewed by the surgeon?
You will see the surgeon 10 to 14 days after the operation and your dressings will then be removed. The wounds will be healed by that time and your stitches will be removed.
Are there things that I should avoid?
Generally there are no restrictions to movement in any direction, just be guided by pain.
You will be encouraged to use your arm normally below shoulder height. Gradually the movements will become less painful. Avoid heavy lifting for 3 week.Be aware that activities at or above shoulder height stress the area that has been operated on. Do not do these activities for 3 weeks.
Try and keep your arm out of positions which increase the pain.
How am I likely to progress?
Patients progress at different rates. The discomfort from the operation will gradually lessen over the first few weeks. You should be able to move your arm comfortably below shoulder height by 2 – 4 weeks and above shoulder height by 6 weeks. The things that take the longest to improve are night pain, being able to sleep on that side and getting your hand up your back. Complete relief pain may take up to 6 months (80% of people have complete relief by 6 months according to research). However, there may be improvements for up to 1 year.
When can I return to work?
This will depend on the type of work you do. If you have a job involving arm movements close to your body you may be able to return within a week. Most people return within 2 weeks of the operation but if you have a heavy lifting job or one with sustained overhead arm movements you may require a longer period off work. Please discuss this further with the surgeon or physiotherapist if you feel unsure.
When can I participate in my leisure activities?
Your ability to start these activities will be dependent on pain, range of movement and strength. Nothing is forbidden, but it is best to start with short sessions involving little effort and then gradually increase the effort or time for the activity. However, be aware that sustained or powerful overhead movements (e.g. trimming a hedge, some DIY, racket sports etc.) will put stress on the subacromial area and may take longer to become comfortable. You may be unable to do these for 4 months post operation.
When can I drive?
You can drive as soon as you feel able. This is normally within 2 weeks. Check that you can manage all the controls and it is advisable to start with short journeys.
Surgery procedure
Shoulder Arthroscopy
Most surgical procedures of the shoulder are now performed with arthroscopy. This involves the inserting of a telescope (fibre optic) through a thin tube in small incisions around the shoulder. The incisions are between 0,5 to 1,0 cm in size and between 2 and 6 incisions are used depending what operation is done. A single stitch or suture is used to close the incisions after the operation.
This is less invasive but the operation inside is the same as those done with an open operation and thus recovery may still take months depending on the procedure performed.
ARTHROSCOPIC PUMP
To facilitate the arthroscopic (keyhole) surgery, fluid is pumped into the shoulder. This opens the spaces in the shoulder and prevents bleeding. During the procedure some fluid leaks into the tissues around the shoulder which can become very swollen. This fluid is absorbed over the following few hours and patients may find that they pass more urine during this period as this fluid is excreted. Some of this fluid which is blood stained leaks out the small incisions and an absorbent dressing (nappy) is strapped to the shoulder. This is left on overnight and is replaced with small waterproof dressings the next morning so that the patient can shower normally.
This bloody fluid tracks down between the skin layer and muscle and patients may develop quite marked bruising down their arm and over their chest/breast during the week following the operation. This bruising will disappear over 2 -3 weeks.
ANAESTHESIA
This is done with a general anaesthetic and a regional block. It can be done with a block alone but the patient is placed into a seated position on the operating table which can be uncomfortable and thus a general anaesthetic is preferred. The block is done with local anaesthetic injected into the side of the neck where the nerves to the arm are passing. This provides excellent pain relief during the operation thus less anaesthetic drugs are required, patients thus wake up quite refreshed afterwards. The block provides excellent relieve of pain after the operation and lasts for between 8 and 24 hours. The arm may be completely dead and the patient may not even be able to move their fingers initially. Care must be taken not to put anything hot on the arm as this will not be felt and a burn may occur. In approximately 1% of cases there may be a persisting area of numbness in the arm, forearm or hand which usually disappears within 3 months. Occasionally neuralgia (nerve pain) may occur after the block and may require medication till it settles of its own accord.
HOSPITAL STAY
Patients come in on the day of the operation and may be discharged a few hours after the operation or may stay overnight depending on the operation performed and how they are feeling.
MEDICATION
An anti-inflammatory and a pain killer are prescribed. The anti-inflammatory is taken for a week and the pain killer if and when necessary. Most patients take the pain killer for an average of 5 days after the operation. Some patients however don’t take any medication whereas other patients may need pain killers for up to 6 weeks. This is dependent on the individual and the operation performed. More pain is usually felt following a rotator cuff repair. Patients often struggle to sleep initially and a sleeping tablet may be required.
SLEEP
Patients often have difficulty sleeping and besides taking sleeping tablets, sleeping propped up with pillows or sleeping in a chair will be easier. A recliner (lazy boy chair) will often be the best option.
Anaesthesia
The anaesthetist will see you in the ward prior to the operation or in the reception room in theatre. If you have medical problems; eg: heart condition, previous cardiac surgery, chest disease (eg: emphysema), you will be referred to a physician for an assessment and may see the anaesthetist a few days prior to the operation. A premed is sometimes given prior to theatre which will make you a little drowsy and relaxed. In theatre you will sit on the theatre table and make yourself comfortable prior to the induction of anaesthesia. A drip will be inserted into your arm through which the anaesthetic drugs are administered. Gases will be given by a mask and once you are asleep a tube will be inserted into your throat, this is why you may have a sore throat for a short time after the operation.
The anesthetic is a general anaesthetic with a regional block. It can be done with a block alone but you are placed into a seated position on the operating table which can be uncomfortable and thus a general anaesthetic is preferred. The block is done with local anaesthetic injected into the side of the neck where the nerves to the arm are passing (essentially an epidural of the arm). This provides excellent pain relief during the operation thus less anaesthetic drugs are required; you tend to wake up quickly and are quite refreshed afterwards. The block provides excellent relieve of pain after the operation and lasts for between 8 and 24 hours. The arm may be completely dead and you may not even be able to move your fingers initially. Care must be taken not to put anything hot on the arm as this will not be felt and a burn may occur. In approximately 1% of cases there may be a persisting area of numbness in the arm, forearm or hand after the block has worn off. This numbness will usually disappear within 3 months. Occasionally neuralgia (nerve pain) may occur after the block and may require medication till it settles of its own accord. Although extremely rare, permanent nerve damage has been reported.
You tend to wake up very quickly after the operation and may eat soon afterwards. The drip will be taken down when you are back in the ward. The block provides excellent pain relief for between 8 and 24 hours but pain killers and anti-inflammatories are started before the block wears off so that they are already working when the pain starts. Patients vary in the amount of pain killers that they need; some don’t need to take any whereas others may need to take them for up to 6 weeks.









